Introduction
Contact lenses (CLs) are widely used for vision correction, with more than 140 million users worldwide, owing to their functional and cosmetic benefits (1). The growing demand for comfortable and cosmetically appealing alternatives to spectacles has further increased their popularity. However, this rise in usage has also highlighted a critical challenge: ensuring proper compliance with contact lens care, particularly with storage case hygiene (2).
Compliance in the context of CL use refers to the extent to which wearers adhere to recommended protocols for cleaning, storage, and maintenance, as advised by eye care professionals. Despite receiving instructions, both adult and younger users often exhibit poor adherence due to negligence, misunderstanding of guidelines, or irregular wear patterns (3). This non-compliance substantially elevates the risk of ocular complications such as microbial keratitis (MK), contact lens peripheral ulcers (CLPU), and contact lens-induced acute red eye (CLARE). Importantly, the contact lens storage case (CLSC) itself serves as a major reservoir for microbial contamination, with studies reporting contamination rates between 58% and 85%, even among asymptomatic wearers. Pathogens such as Pseudomonas aeruginosa, Serratia marcescens, Staphylococcus aureus, fungi, and Acanthamoeba are commonly isolated from CLSCs (4).
Previous studies have documented that 40–91% of lens wearers demonstrate non-compliance with care and hygiene practices, depending on factors such as lens type, replacement schedule, and cleaning regimen. Notably, up to 80% of CL-related complications are considered preventable through proper adherence to hygiene and storage practices (5). These findings underscore the importance of consistent patient education and effective communication from practitioners to improve compliance levels.
Against this background, the present study focuses specifically on CLSC hygiene, an area often overlooked despite its critical role in preventing infections. The study evaluates cleaning routines, replacement frequency, and storage methods among CL wearers visiting a tertiary eye care hospital. Furthermore, it examines the type of instructions provided by eye care professionals and assesses the level of awareness and perceived risk among users. By doing so, this study adds to existing literature by providing insights into real-world compliance patterns in an Indian tertiary care setting, helping to identify gaps that can be targeted through improved patient education and counseling.
Methodology
Ethical approval for this study was obtained from the Institutional Review Board of Sapthagiri Institute of Medical Sciences and Research Center (Ref No: SIMS & RC/EC-14/Stu-09/2024-25). The study was conducted in the contact lens department of the same institute between August and November 2024. The target population comprised contact lens users attending a tertiary care hospital. A total of 103 participants were enrolled in this cross-sectional study. Individuals using daily disposable CLs were excluded, as they do not require storage cases. Only responses from non-daily disposable lens wearers who owned a storage case were included in the final analysis.
A custom-designed, self-administered questionnaire was developed using Google Forms. The questionnaire was structured into five sections.
The first section gathered demographic information, including age, gender, and educational background. The second section addressed general aspects of CL use, such as lens type, usage patterns, replacement schedules, duration of wear, care products used, and purchase behaviors. Participants using daily disposable lenses were instructed to discontinue the survey and were excluded from the study. The third section focused on CLSC practices, including cleaning methods, drying habits, replacement frequency, solution handling (e.g., topping off), and storage location. The fourth section examined the participant–practitioner relationship, specifically whether oral and/or written instructions on CLSC maintenance were provided and if written guidance was later reviewed. The final section explored participants’ perceptions of the consequences of poor storage case hygiene and their risk assessment of non-compliant behaviors, rated on a scale from 1 (no risk) to 5 (maximum risk).
Participants were informed about the study’s purpose and assured that participation was voluntary, with the option to withdraw at any stage without consequences. A patient information sheet was provided prior to enrollment, and informed consent was obtained online. The questionnaire was distributed via Gmail, WhatsApp, Facebook, and Instagram and was available in both English and Kannada. Participants were requested to complete the form within the Contact Lens Outpatient Department (CL OPD).
Data recorded electronically were transferred to Microsoft Excel for processing. Categorical variables were summarized using frequencies and percentages. Nonparametric analysis was used for statistics, and P-values were calculated using statistical package for social science (SPSS) (version 20). A P-value ≤ 0.05 was considered statistically significant.
Results
Survey response
The study achieved a 100% response rate, with all 103 eligible participants completing the survey and providing informed consent to participate.
Demographic details
Participants ranged in age from 16 to 32 years, with a mean age of 24.68 ± 3.33 years. The majority was female (72 participants; 69.9%). Most respondents held an undergraduate degree (73; 70.9%). Regarding contact lens experience, 56 participants (54.4%) had been wearing lenses for less than 1 year, while 44 (42.7%) had between 1 and 5 years of wearing experience.
Contact lens type, replacement modality, usage, and lens care solutions
Silicone hydrogel soft lenses were the most commonly used type (66 participants; 64.1%), followed by hydrogel soft lenses (23; 22.3%). The most frequently reported replacement schedule was monthly (59; 57.3%), likely due to factors such as convenience and cost-effectiveness. Most participants reported daily use of their lenses (91; 88.3%), either full-time or part-time. In terms of lens care, the majority used multipurpose solutions (MPSs) (81; 78.6%), followed by peroxide-based solutions (21; 20.4%).
Table 1 provides a summary of demographic details, as well as contact lens type, use and replacement, wearing experience, and type of contact lens solutions reported by the participants.
Contact lens storage case practices
A majority (81; 78.6%) reported cleaning their lens case, while 22 participants (21.4%) did not clean it at all. Among those who did clean their case, 10 (9.7%) cleaned it daily, 22 (21.4%) once a week, 65 (63.1%) used MPS, and 19 (18.4%) used soap and water. Approximately one-third (34; 33.0%) dried their case with a disposable tissue, while 20 (19.4%) refilled the case with solution without drying it. Regarding replacement practices, 26 participants (25.2%) replaced their case every 1–3 months, 19 (18.4%) monthly, and only 7 (6.8%) replaced the case with each new solution bottle. Most participants (39; 37.9%) refilled the case only when the solution level was low, whereas 35 (34.0%) replaced the solution daily. When lenses were left unused in the case for several days, 50 (48.5%) admitted they never changed the solution, 43 (41.7%) did so every 1–2 weeks, and only 10 (9.7%) reported changing it daily. In terms of storage location, 35 participants (34.0%) kept the case in a cupboard, 34 (33.0%) on a table, and 10 (9.7%) stored it in the washroom.
Table 2 illustrates the frequency of self-reported case hygiene and replacement practices.
Relationship with eye care professionals
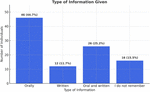
The majority of participants (96; 93.2%) reported receiving instructions from their eye care professionals regarding case cleaning and replacement. Of these, 46 (44.7%) received only oral instructions, 12 (11.7%) received only written information, and 26 (25.2%) received both as described in Figure 1. However, of the 38 who received written instructions, 33 (32.0%) admitted they did not refer to them at home. When asked about the consequences of poor storage case hygiene, 84 participants (81.6%) recognized an increased risk of infection, while 13 (12.6%) cited discomfort. Regarding purchasing behavior, 36 (35.0%) obtained their lenses from a different optical or vision center, 24 (23.3%) purchased lenses from the same place they received their prescription, and 5 (4.9%) purchased them online.
Perceived risk of noncompliant practices
Participants’ perceived risk scores (on a scale of 1–5, where five indicates maximum risk) for three noncompliant behaviors: not washing hands with soap and water, infrequent cleaning of the storage case, and infrequent replacement of the case, as demonstrated in Figures 2, 3, and 4, respectively. Overall, participants demonstrated a high level of risk awareness, with median scores of 4 or 5. Female participants associated greater risk with inadequate hand hygiene (P = 0.008) and infrequent case cleaning (P = 0.02). Similarly, those with higher educational attainment perceived a greater risk from poor hand hygiene (P = 0.03) and inadequate case cleaning (P = 0.03). Increased years of contact lens use were significantly associated with higher risk perception for improper hand washing (P < 0.001), but not for storage case maintenance. Participants who received explicit instructions from their practitioners assigned higher risk to infrequent case replacement (P = 0.01), with no significant difference between those who received only oral and those who received both oral and written guidance.
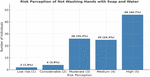
Figure 2. Participant’s response regarding risk perception of not washing hands with soap and water (1: Low risk; 5: High risk).
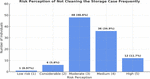
Figure 3. Participant’s response regarding risk perception of not cleaning the storage case frequently (1: Low risk; 5: High risk).
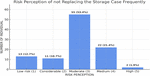
Figure 4. Participant’s response regarding risk perception of not replacing the storage case frequently (1: Low risk; 5: High risk).
Discussion
A total of 103 participants were included in this study, with a majority being female (69.9%). The age range was 16–32 years (mean: 24.68 ± 3.33 years). A self-reported survey was utilized to assess compliance with hygiene and replacement practices of CLSCs among users attending a tertiary care hospital.
Consistent with findings by Gammoh et al. (6), MPSs were the most commonly used care product in this study, reported by 78.6% of participants. MPS is often preferred for its ease of use, convenience, and cost-effectiveness, as it combines cleaning, rinsing, and disinfection in one solution.
Regarding contact lens case hygiene, 78.6% of respondents reported cleaning their cases; however, only 9.7% cleaned them daily, 21.4% weekly, and 17.5% monthly. Notably, 21.4% never cleaned their cases, a practice known to contribute to microbial contamination, as highlighted in previous studies (6). Similarly, Gammoh et al. (6) reported a 76.5% contamination rate associated with poor cleaning habits.
Unlike Cardona et al. (7), who found that a majority stored their lens cases in bathrooms—environments prone to contamination—this study found that participants commonly stored their cases in cleaner environments, such as cupboards (34%), tables (33%), or bedrooms (8%), with only a small proportion using bathrooms (2%) or washrooms (10%). This suggests a relatively better awareness of hygienic storage practices among our participants.
Compared to a study by Zainodin et al. (8), which reported 52% non-adherence to lens care among young users, our findings show a higher rate of moderate compliance (68%) among participants aged 16–32. Furthermore, it also reported a 48% non-compliance rate; our study found a significantly lower rate (2.9%), reflecting greater awareness of the risks associated with poor hygiene, such as bacterial keratitis, corneal ulcers, fungal or amoebic infections (e.g., Acanthamoeba), and oxygen deprivation-related complications.
All participants owned their own CLSC, suggesting access to appropriate lens care tools. However, lens case replacement practices remained suboptimal. Only 19.4% replaced their cases when damaged, lost, or visibly dirty, and 3.9% never replaced them—supporting prior findings by Madhavendra et al. (9) and Thakur et al. (10) on the role of contaminated cases in MK.
Thakur et al. (10) also reported a higher rate of MK in low-compliance groups (P < 0.05). In our study, moderate awareness of CLSC-related risks was observed. While only 11.7% perceived poor cleaning as high risk, 35.0% rated it as medium and 46.6% as moderate risk (P = 0.527). This highlights the need for reinforced education on the importance of consistent case hygiene to prevent avoidable complications.
Conclusion
In conclusion, the findings indicate moderate awareness among contact lens users regarding the risks of improper lens and storage case care, though gaps in practice persist. While many participants acknowledged the importance of hand hygiene, regular cleaning, and timely case replacement, fewer recognized these behaviors as high-risk, suggesting an underestimation of potential health consequences. Although general knowledge exists, consistent adherence to recommended practices appears limited. These results underscore the need for targeted patient education by eye care professionals, reinforcing the importance of proper hygiene and maintenance to prevent infections and enhance ocular health among contact lens wearers.
Funding
None of the authors have reported funding/support.
Acknowledgments
The authors want to acknowledge Genis Cardona, author of the study “Compliance versus risk awareness with contact lens storage case hygiene and replacement,” for her approval to use the questionnaire for the present study.
The authors also like to acknowledge all the respondents for their active participation in this study.
Finally, the authors used the ChatGPT 4.0 AI tool to improve the language and readability of the texts.
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
References
1. Tüfekçi Balıkçı A, Cazımoğlu İ, Yalnız Akkaya Z, Burcu A. Compliance of hospital healthcare professionals with contact lens use and care. Kırıkkale Uni Med J. (2024) 26(1):91–9.
2. Pucker AD, Tichenor AA. A review of contact lens dropout. Clin Optom (Auckl). (2020) 25(12):85–95.
3. Beshtawi IM, Qaddumi J, Suboh N, Zaid A, Mansour H, Zeyadeh T. Compliance of soft contact lens care and bacterial contamination among university students in Palestine. Clin Ophthalmol. (2022) 16: 4121–34.
4. Kumar R, Gupta D. Awareness and compliance in contact lens wearers: case study. J Multidiscip Res Healthcare. (2018) 5:33–7.
5. Stapleton F, Keay L, Edwards K, Naduvilath T, Dart JK, Brian G , et al. The incidence of contact lens-related microbial keratitis in Australia. Ophthalmology. (2008) 115(10):1655–62.
6. Gammoh Y, Asfour W. Compliance to contact lens wear and care among Jordanian adults. PLoS One. (2023) 18(1):e0280409.
7. Cardona G, Alonso S, Yela S. Compliance versus risk awareness with contact lens storage case hygiene and replacement. Optom Vis Sci. (2022) 99(5):449–54.
8. Zainodin EL, Abdul Hadi NS. Non-compliance behavior in contact lens wear and care among university students. Environ Behav Proc J. (2020) 5(14):11–8.
9. Bhandari M, Hung PR. Habits of contact lens wearers toward lens care in Malaysia. Med J Malaysia. (2012) 67(3):274–7.
10. Thakur DV, Gaikwad UN. Microbial contamination of soft contact lenses & accessories in asymptomatic contact lens users. Indian J Med Res. (2014) 140(2):307–9.
© The Author(s). 2025 Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.